

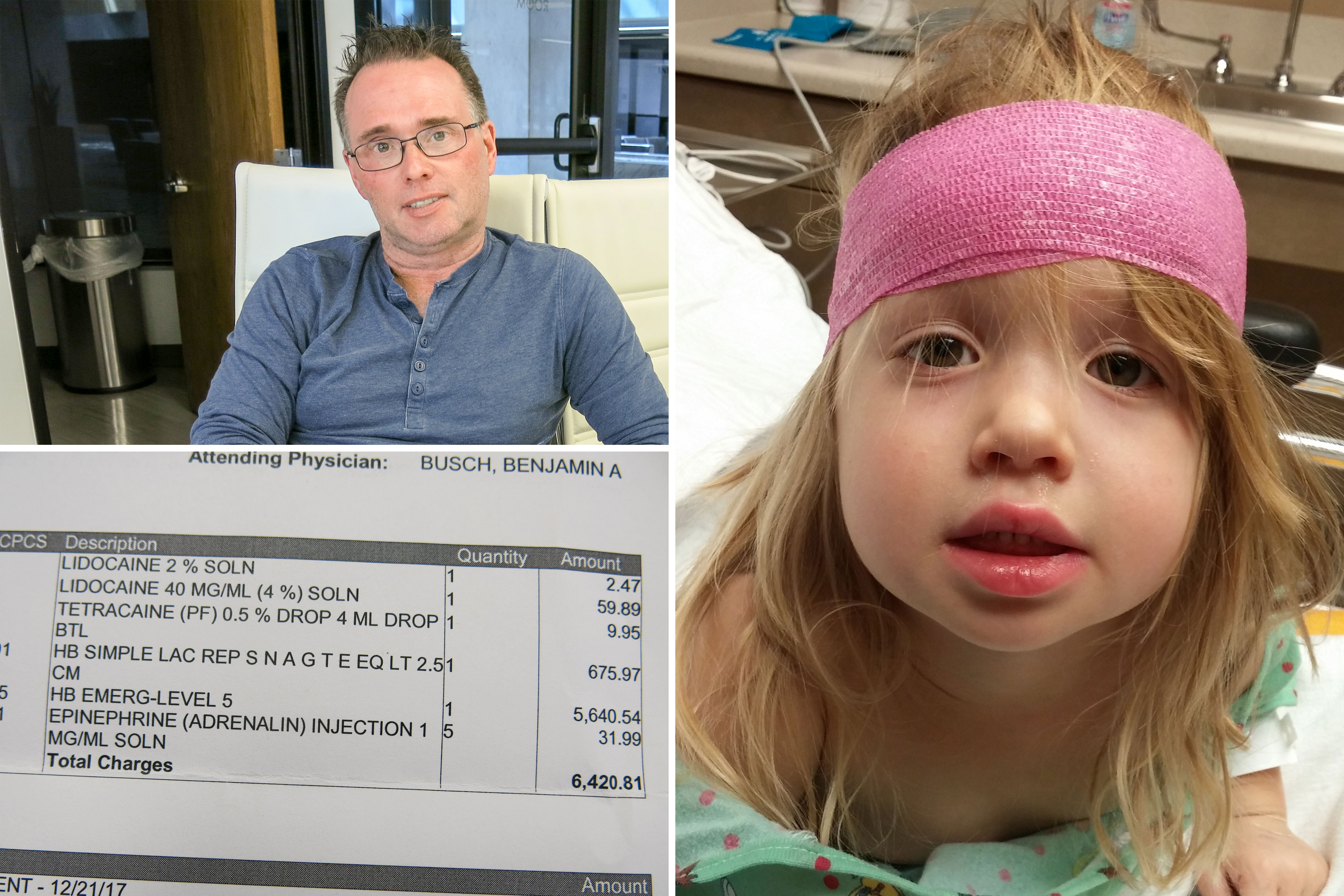
Ken Wehking’s three kids were horsing around last Thanksgiving when two-year-old Kelseigh took a tumble. The back of her head found the coffee table, opening up a wound that needed treatment.
Google Maps told Wehking the nearest urgent care was a facility in a nearby Arvada shopping center. It was his impression that insurance would cover most of the claim — then he got the bill.
“I was shocked,” he said. “It was $6,400. And I'm like ‘what is this for?’”
The bulk of that total was a single medical charge of $5,600 for the emergency visit. Wehking is a health analyst professionally and he said it “was a sticker shock.” If he’d have known, he would have gone elsewhere.
It's stories like this that prompted three bills in Colorado’s Legislature to rein in freestanding emergency rooms: One is a bill that requires posting of consumer notices, another regards reimbursement from insurers and the third is a requirement to license these kind of health facilities. Rep. Lang Sias, a cosponsor of two of the bills and a Republican from Arvada, said “consumers get this at a very at a very gut-level.”
Sias sees himself a free market conservative, but said markets don’t work well if people don’t have information like basic pricing.
“Be in business, charge what the customers are willing to pay, but you’ve got to be transparent so that they can make decent decisions,” Sias said.
Democratic Sen. Irene Aguilar, a medical doctor who represents Denver, offered a prescient warning about costs at these kind of facilities way back in 2014.
“The concern was that this was going to be a new business model. And how could we stop this in its tracks?” Aguilar said. “I could see how it was going to be ripe for abuse.”
She tried to ban them within 25 miles of hospitals. She tried to prevent them from charging facility fees. Aguilar had seen them spread like wildfire in Texas and anticipated it would happen here. “And unfortunately that was exactly what happened.”
Her legislative proposals went nowhere. At the time there were 15 freestanding ERs in Colorado. Now there are more than 50. One reason is that Colorado is one of a few states that don’t require a certificate of need, sign off from the state about whether local demand is enough, to build a new facility. That means they can go up anywhere, competing for patients.
Edmond Toy of the nonpartisan, nonprofit Colorado Health Institute pointed out that these are “emergency rooms and they charge emergency room prices.” And like Ken Wehking’s reaction to his bill, “a lot of people aren't expecting that.”
The Colorado Health Institute has a complete list of freestanding ERs in the state. Only Texas and Ohio have more, Toy said. There are now more than 500 around the nation.
Many have sprung up in affluent suburban communities along the Front Range, often in areas where patients have less urgent medical conditions and good insurance. Consumers like the convenience, but balk at what looks like price gouging. Now lawmakers of both parties are taking notice.
“The fact that this is the first year where these kinds of bills have gotten this far in the legislative process is reflective of that tension I think,” Toy said.
Legislative proposals aimed to boost transparency regarding the facilities have gone nowhere in recent years. But during the 2018 legislative session, Colorado lawmakers have started to make some headway.
The first bill, SB 18-146, would make freestanding emergency departments post prices on the 25 most common healthcare services provided. It would also require facilities give consumers a written statement saying they’ll be screened and treated regardless of ability to pay, as federal law requires.

The legislation also requires the facility to state if it only provides emergency care, or if it provides both urgent and emergency care. And it would require facilities specify which insurance plans are in or out-of-network. The bill has passed both chambers and is on the way to the governor’s desk.
“I think it's a step in the right direction for sure,” said Jennifer Risdon, a mother in Arvada. A couple of years ago, she took her then 12-year-old son Gavin to a Centura Health facility near her home for a sore throat. She checked ahead to make sure the facility was in her insurer’s network. It was. Gavin was given a strep test, and Risdon said a doctor looked at him for a few minutes.
Later the bill came. She described her reaction as “You gotta be kidding me, $841 for five minutes!”
It turned out the facility was in-network, the doctor was not. Risdon eventually was able to get the fee waived, but “it was a nine-month ordeal and it took a lot of diligence.”
Jennifer Wills, corporate communications director for Centura Health, described that situation, where a patient gets charged for being treated by an out-of-network doctor at an in-network facility, as “rare.” She said this should be transparent to the consumer.
“Consumers should not have to guess if a provider is in-network or out-of-network at an in-network facility,” Wills said. “We have and will continue encouraging our aligned physician providers to be contracted and in-network with our payer partners.”
Reimbursement from insurers is addressed in the second bill, HB 18-1282. It requires the freestanding emergency facilities to identify themselves separately from hospitals when looking to get reimbursed for services. This would enable costs for care at the facilities to be compared with traditional hospital emergency departments.
Like the Senate’s transparency bill, this House bill on facility identification has passed the legislature and awaits the signature of Gov. John Hickenlooper.
The third bill has made little progress under the gold dome. HB 18-1212, which is opposed by the Colorado Hospital Association, would create a new license for these type of facilities.
Freestanding ERs are also getting pushback from the advisers to a powerful federal insurance agency: Medicare. A recent proposal from the Medicare Payment Advisory Commission, which reports to Congress, could impact their bottom line. It would cut Medicare payment rates 30 percent on some services at facilities located within six miles of an emergency room within a hospital.
The facilities are usually owned by or are affiliated with hospitals. Julie Lonborg, vice president of communications and media relations with the Colorado Hospital Association, said they’ve heard complaints from customers, and her organization along with its member hospitals “are absolutely committed to further transparency around freestanding emergency departments.”
She said the CHA is recommending hospitals post information about pricing and facility fees. They’ve also created a consumer-focused campaign and website, called Where for Care, about when to use primary, urgent or emergency care. Lonborg does point out that consumers want quality care close to home, without a wait, and these systems meet that desire.
“I think that's the model of the future nationally and for Colorado,” Lonborg said.
UCHealth has a number of freestanding ERs and has been adding more. Spokesman Dan Weaver said it offers a variety of services and has worked to educate patients about the difference. Emergency departments are the most expensive form of care, and Weaver said if patients have a problem that can be handled outside of emergencies, they should “utilize the urgent care or primary cares first.”
It was an UCHealth facility that treated Ken Wehking’s daughter and sent him the bill for more than $6,400. Weaver can’t talk about a specific case, but said hospitals offer discounts based on contracts with insurers. They also provide discounts for self-pay patients or the uninsured.
“So, it's important to look at the actual billed amount that comes after that discount,” Weaver said.
Ultimately, Ken Wehking’s insurance covered most of the surprise ER bill. But he wonders if the facilities can survive full cost transparency.
“They would probably end up having to shut down, because I don't think people would be using them very often,” Wehking said.
Consumers will get a look at the new rules soon. If the governor signs the transparency legislation as expected, they could see the new notices next year.








