As the coronavirus pandemic continues to exact a toll on Colorado in the form of lives and economic damage, it’s an intense time to graduate from college. Let alone a nursing school.
Yet, this moment is exactly where the class of 2020 finds itself.
One of those future front line professionals, self-described “baby nurse” Anna Gordon-Norby, of Aurora, wants nothing more than to be a corrections nurse. Jails and prisons are one of the places, alongside nursing home facilities, that have become breeding grounds for COVID-19.
“It's such a disenfranchised or underrepresented community that, you know, my little social work-y [sic] heartstrings are drawn to it,” she said.
You might say nursing is the family business. Gordon-Norby’s father and grandmother were nurses. The graduate of the University of Colorado College of Nursing has already had several job interviews.
“The thought of joining correctional nursing right now, during a pandemic, I guess it's terrifying. Because everyone is in such close quarters and so that's scary. But then also I would be proud to be able to jump into that response,” she added.
At Colorado Matters’ request, Gordon-Norby agreed to a video chat with a veteran nurse who might offer insight into the profession during a global health crisis. Erin Kunkel of Swedish Medical Center in Englewood was thrilled to participate.
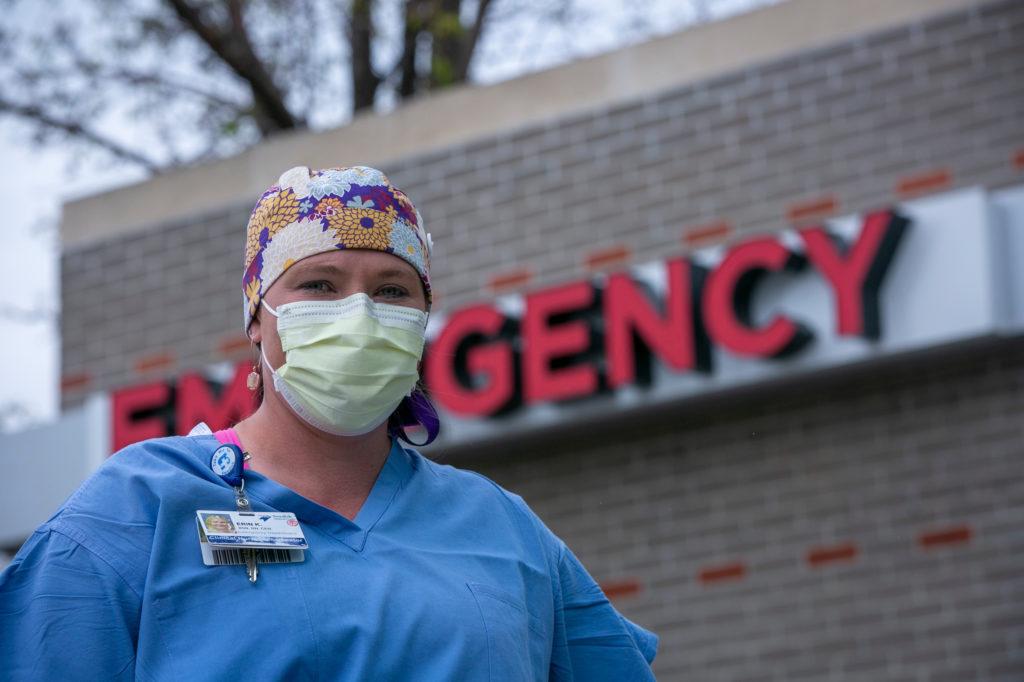
“Growing new nurses and mentoring them is one of my passions,” she told Gordon-Norby. “I'm really excited for you and truly the whole class of 2020. How exciting it is to be a nurse and come into health care in a moment like this!”
Kunkel, a 16-year veteran at Swedish, is a clinical nurse coordinator and charge nurse in the emergency department. Here are some of Gordon-Norby’s questions about being a nurse during a pandemic and Kunkel’s answers.
What has been your greatest challenge in nursing?
“Honestly, the biggest challenge clinically in my whole career has been right now caring for these patients through COVID — when we are turning visitors away at the door for their safety and ours. I have to look a family member in the face and tell them ‘we're going to do the best we can to care for your loved one’ and then take their phone number. I think that has been the absolute hardest because when you are in a health care situation, you want your loved ones with you. And as the nurse, I want them to have their loved ones with them! So that has definitely been the hardest clinical situation is not having family members at the bedside.”
What advice would you have for a ‘baby nurse’ entering the field right now?
“Currently, a lot of nurses are coming from other floors as some units are closed or they're reallocating resources to where they need to be. A lot of them are ‘baby nurses.’ So just being open and flexible to really meet the needs. Wherever they put you, you really are making a difference.
“In the ER, it’s unpredictable how many patients come in the door. You know, they don't make appointments. Sometimes we just get crushed when they all show up at the same time. So sometimes taking just three minutes to step outside and take a breath of fresh air will help recharge and make me be able to reprioritize what I need to get done and do it way more efficiently. Take that self-care time, three minutes, maybe even 60 seconds, and think through ‘I am proud to be here. I'm happy to be here and together as a team we can do this.’ ”
What is your greatest accomplishment in patient care?
“I work at a stroke center and strokes are definitely my passion. A couple of years ago, I remember taking care of a patient that had come in for something completely unrelated, maybe belly pain. I had walked into the room and the patient had right-sided paralysis and I was able to notify our stroke team immediately. We took this patient over to get pictures of their head and then we were able to give the drug TPA to help bust up the clot they found in his brain. This gentleman made a complete and full recovery. He was married, had two young kids.
“And I always say ‘make a connection early with your patients.’ Caring for them like you would your family. Sometimes you just don't think you have time to go grab that blanket or you don't have time to get that one thing that they need. But you sure would make time if it was your mom!”