
Owetta McNeil, 82, does not like it when people mispronounce her name.
“It’s ‘OH WEE-TAH’ she admonishes, making sure people know her name should be pronounced with double “e” sound.
McNeil, who worked as a secretary for Denver Public Schools for more than 30 years, has lupus, leukemia along with several other medical conditions, and speaks haltingly after a stroke in March.
Her age makes her especially susceptible to complications from the coronavirus, as does her race. McNeil’s mother was Black. Her father was part American Indian. In Colorado, people of color are disproportionately likely to be hospitalized due to the virus.
Even so, McNeil wasn’t sure what she’d do when doctors advised her to get the COVID-19 vaccine.
“I thought I might chicken out,” she said.
Her reasoning dates back hundreds of years to a distrust of the government. The problem still persists today: People of color have long received subpar medical treatment and worse, have been subjected to abuse by the medical system.
“I was very, very hesitant as a person of color to be involved with vaccines,” McNeil said. “We’ve always been used as experiments and most people my age especially recall what occurred.”
She points to the “Tuskegee Experiment,” a study to determine the effects of untreated syphilis, where Black men in Alabama were recruited and unknowingly denied treatment for the disease, even when penicillin became available to treat it. The study spanned 40 years and at least 28 men died, though experts believe the death toll was much higher.
A study by the Pew Research Center found that Black Americans are less inclined to take the COVID-19 vaccine compared to whites or Latinos.
Over 60 percent of whites and Latinos say they definitely or probably would get vaccinated, while just over 40 percent of Blacks said they planned to.
McNeil specifically doesn’t trust the government to develop a vaccine that protects Black and brown people. She even speculates, based on that sordid history, that Blacks could be given a different — perhaps risky — version of the vaccine from whites, even though there’s no evidence that would happen.
Yet, on Jan. 22, McNeil put her fears aside and pulled up to a drive-through vaccine clinic at National Jewish to get her first dose of Pfizer’s COVID-19 vaccine. After, she waited in her car for the required 15 minutes to make sure there were no side-effects. She was pleasantly surprised to discover that she felt absolutely fine.
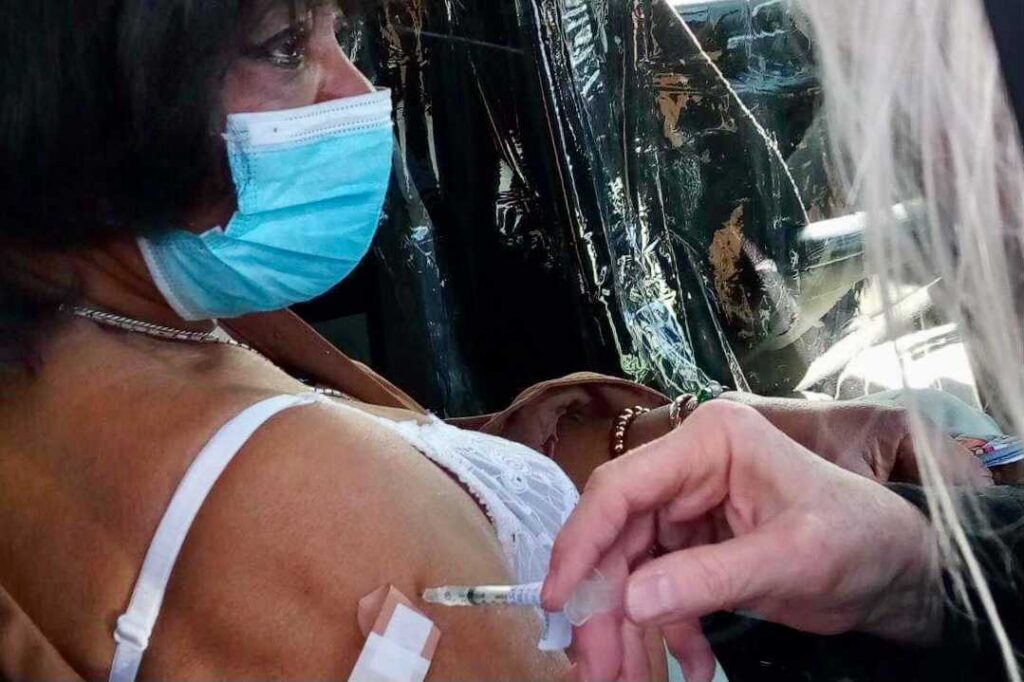
“I'm still here,” she said, adding that she plans to take the second dose of vaccine soon. “And if I have any ill-effects after the vaccine is done, I will just say, that's my contribution to my people.”
Provided those ill-effects don’t materialize after that second dose, McNeil said her goal will be to get her Black friends who don’t plan to get the vaccine to change their minds.
There is one person, however, that McNeil is unlikely to convince: her daughter, Lisa Pitts, who’s a nurse in Denver.
She said, like her mom, she doesn’t trust the government and in this case, the herculean effort to develop and approve a coronavirus vaccine.
“It was pushed through so fast,” she said. “They don’t know how it’s going to affect your immune system or if you’re still of age where you can have kids, how it’s going to affect [them]. I just don't have enough information on it to tell me that...it’s going to be safe.”
It's true that vaccines to fight the pandemic were created in record time.
They've also been subjected to rigorous review in nations around the world and so far, side effects from the shots have been mostly minor. No deaths have been directly linked to vaccines, though research is ongoing.
Even though the drug companies have pledged to have diverse pools for the vaccine testing trials, Pitts still has questions about whether enough Black people have been tested.
“How many people of color did [they] actually test it on?” she said. “Because there's not too many of us that are going out there and saying, ‘Oh yeah, try it on me.’”
People of color have a history of being under-represented in drug trials. In recent years, drugmakers have been urged to recruit more Black people and other racial and ethnic groups into studies.
Pitts said she made her decision to forgo the vaccine despite her career as a health care provider and the pressure on nurses and doctors to get vaccinated. Employers have the ability to require vaccinations for those employees who qualify, but few, including the hospital where Pitts works, which she chose not to disclose, have taken that step.
She said the lack of trust Black people have for vaccines extends more broadly to doctors and the health care system overall, which is why many people of color prefer non-white doctors and nurses.
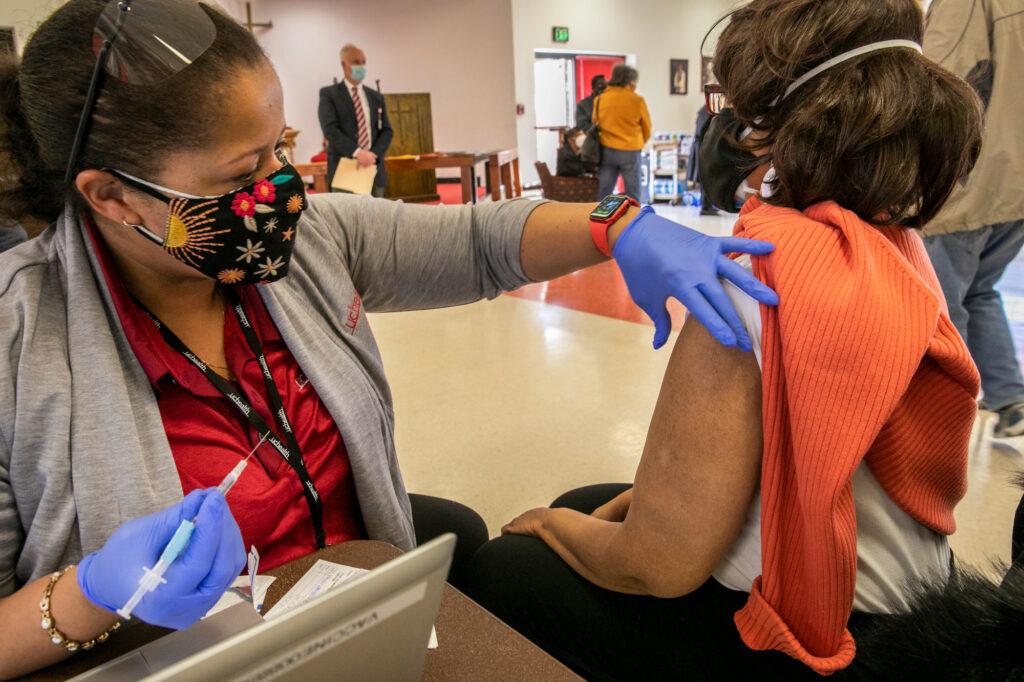
“If you're Black, if you're a minority, then you'd rather go to a minority,” Pitts said. “A lot of white doctors will dismiss you.”
She said her brother was complaining in July about his shoulder hurting and went to the VA for treatment but the doctor wouldn’t give him anything but ibuprofen.
“Finally I told him, you need to put your foot down and tell them you want an X-ray or an MRI,” Pitt’s said. “And he finally did and it ends up he has bone cancer.”
Despite her views, Pitts said her mother, Owetta McNeil, probably made the right decision to get inoculated because of McNeil’s many health conditions.
The isolation due to the coronavirus has been hard at times for McNeil and she misses seeing her friends. There’s one thing in particular she’s determined to do once she’s fully vaccinated. Pre-pandemic she took a tour bus to Black Hawk once a month to go to the casinos. She said she plans to start making those trips again — with a mask and a bottle of hand sanitizer, of course.
“I am sick of sitting around with money in my pocket,” she said.









