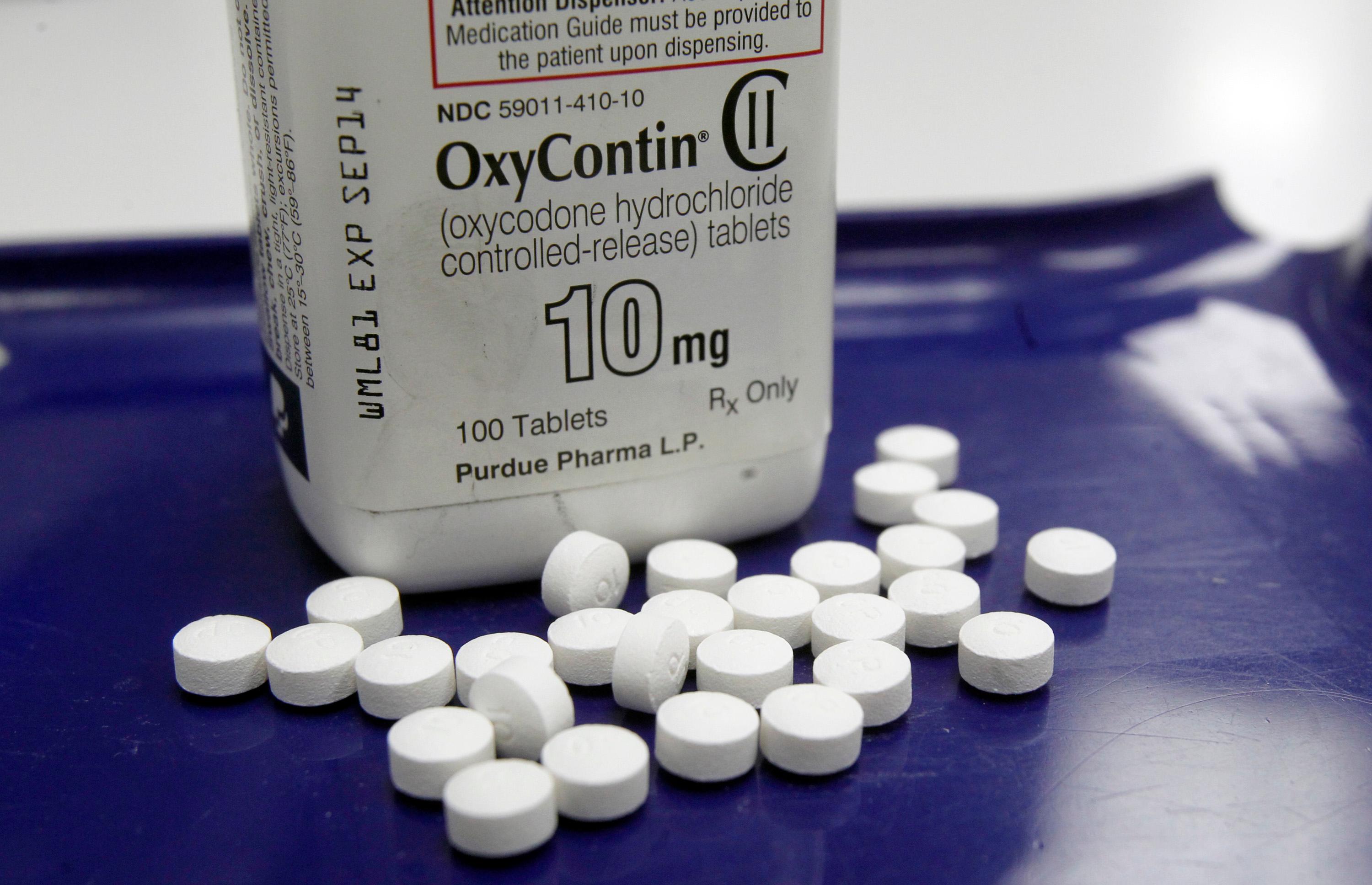
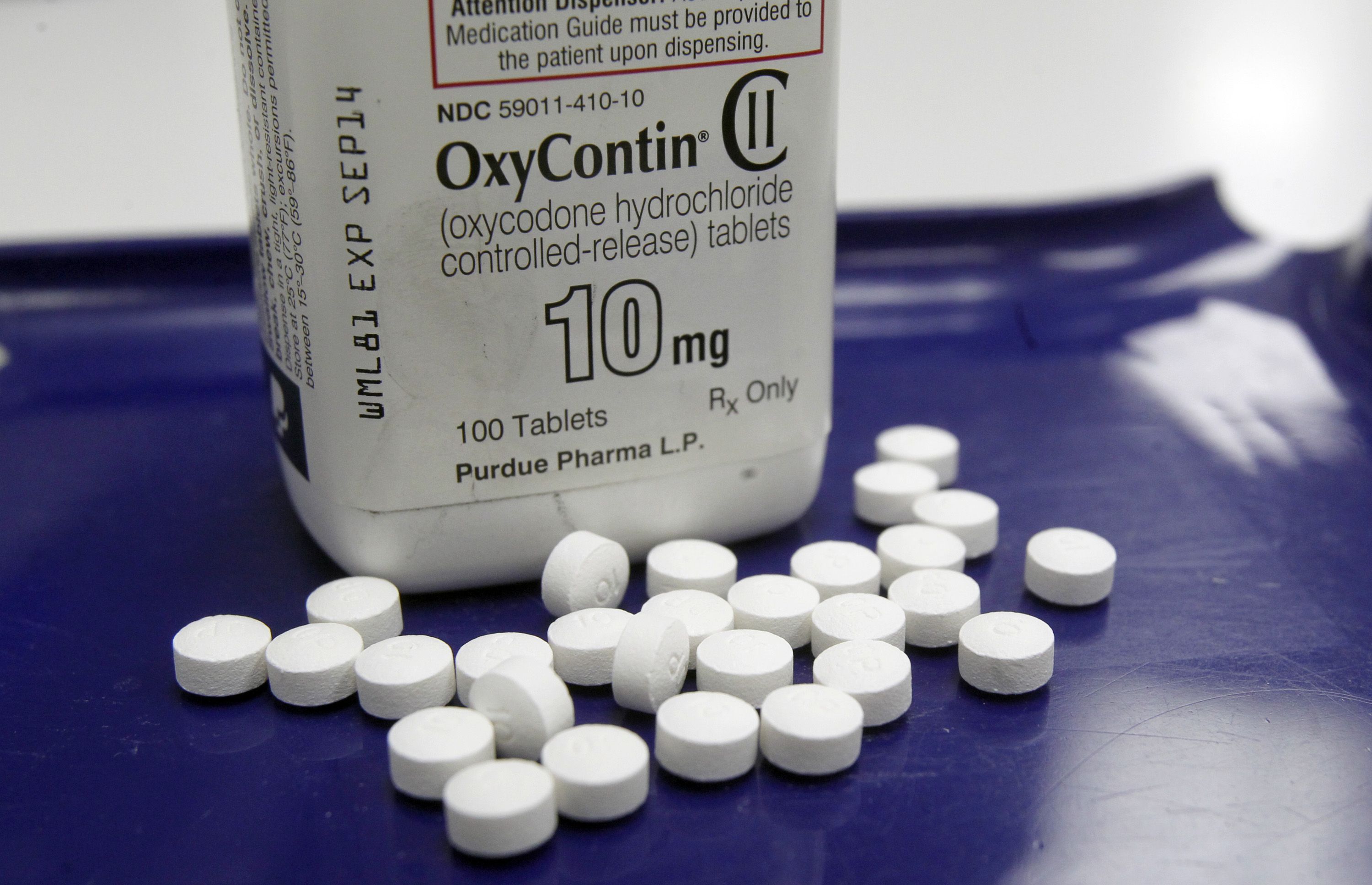
The scale of Colorado’s opioid crisis prompted lawmakers to look at a variety of angles in order to tame the problem. One of the approaches, now sitting on the governor’s desk awaiting a signature, is a bill that limits how much medication a doctor can prescribe in specific situations.
Opioids are primarily prescribed by primary care or emergency department providers. This legislation targets prescriptions for acute pain, which may be more sharp and severe but short-term. Not all doctors though are happy with the move.
Some medical professionals worry the legislation will set a precedent and allow outside forces to intrude on medical decisions.
“I’m against this because I believe in the sanctity of the doctor patient relationship as foundational to the practice of medicine and the decision-making that would follow that,” said Dr. Christopher Unrein, an internist and past president of the Colorado Medical Society.
The measure would restrict the number of opioid pills a health care practitioner, may prescribe — that includes doctors, nurses and dentists. The limit is a 7-day supply on initial prescription, and a refill for a 7-day supply, with some medical exceptions based on a patient’s condition and need.
Supporters point to various studies. One found opioid dependency could develop just a few days after initial use. Dr. Shannon Jantz, with Colorado Academy of Family Physicians, said another study from 2017 showed patients given more opioids with an initial prescription were more likely to develop an addiction.
“We do have some data really saying that if we are better about, on initial prescribing, prescribing less, prescribing more thoughtfully, that we are less likely to create people who are long-term users,” Jantz, a family medicine physician, said.
Proponents point out that the 7-day limit applies just to the initial prescription for acute pain, not for chronic pain or cancer-related pain. The measure will sunset in 2021. Unrein still disagrees, as he said doctors should be able to decide what’s right for a patient, using their knowledge and education.
“You know, where does it stop?” he asked. “When we start regulating and legislating and micromanaging the practice of medicine in the legislature, where does it stop?”
The bill also sets up a report card through the state’s prescription drug monitoring program so doctors can see how they’re doing compared to peers. In an interesting wrinkle, trial attorneys also wanted access to that data. That didn’t come to pass, but Robert Valuck, director of the Colorado Consortium for Prescription Drug Abuse Prevention, said they eventually worked out a compromise.
“My understanding is that the trial lawyers association and the medical society got together basically and they decided how to write protections for doctors that would be acceptable to both sides so that neither one would oppose the legislation.”
Five of six major opioid-related bills got through the 2018 Colorado legislative session. The one that was stopped in its tracks was the Harm Reduction Bill, which would have allowed Denver to press forward with a safe-injection site. The others that made it have to do with prevention, treatment, insurance coverage and expanding the pipeline of providers. Taken as a whole this is the most comprehensive package Colorado lawmakers have passed in response to opioids. Still, there’s a long way to go to tackle this enormous issue.