Updated Jan. 25, 2022
Colorado is a long way from March 2020, when the first two presumptive cases of coronavirus were detected in the state.
There are vaccines that have proven to be highly effective at preventing hospitalizations and death. And there are treatments and therapies for COVID-19 that can be administered in hospitals or before someone even has to go there.
But for those thinking that the availability of these treatments means it’s safe to let their guard down against this deadly virus, Dr. Jaya Kumar, the chief medical officer at Swedish Medical Center, has a stern warning: They aren’t cures for COVID-19, and they don’t always work.
“These therapies exist, but they’re not without risks. They’re not without side effects. They're not 100 percent [effective],” Kumar said. “You could still progress to severe illness and death.”
She adds that getting these treatments after testing positive for coronavirus isn’t as simple as walking into the emergency room or a doctor’s office. Most require special equipment and hours of attention from hospital and medical workers at a time when many of them are feeling burned out, and hospitals are struggling with capacity.
So what are my options before going to the hospital with COVID?
First, you have to know if you actually have COVID-19. Here's a list of places where you can get tested.
If you’ve consulted with your doctor after testing positive for COVID-19, depending on your symptoms and risk of your illness getting worse, they may send you home with over-the-counter medicine and orders to quarantine.
But if they think you’ll get sicker, they may refer you to get a treatment you’ve probably heard about called…
Monoclonal antibody treatment
These are lab-made proteins based on real antibodies from recovered COVID-19 patients. They’re administered through an IV or injection and they’re meant to neutralize the virus early in the course of a COVID-19 case, said Dr. Adit Ginde, emergency physician at UC Health.
It’s important to remember that these are only administered within the first 10 days of symptoms, and they’re most effective within three to five days, Ginde said.
Currently, the treatment is only available to those in high-risk categories like:
- Being 65 or older
- Being overweight
- Having heart or lung disease
Finding the treatment in Colorado has proved a bit difficult. Recently, Gov. Jared Polis issued an order allowing high-risk patients to refer themselves to get the treatment if they need it.
On Jan. 24, the Food and Drug Administration halted the use of two monoclonal antibody treatments — Regeneron and Eli Lilly — because they are not effective against the omicron variant of COVID-19. Their emergency use authorization was also revoked.
So getting monoclonal antibodies will keep me out of the hospital, right?
Maybe. Monoclonal antibody therapy can keep people from needing hospitalization, but Kumar said the effectiveness of different antibody treatments ranges from 50 to 70 percent max based on several independent studies. If it works for you, it may keep you out of the hospital.
If you’re wondering where to get this treatment, the state health department has a list of available centers where you can find it.
So if I end up in the hospital with COVID, how would I be treated?
That depends on a variety of issues like age and being immunocompromised — meaning several conditions like having HIV, cancer, being pregnant or obese, Kumar said.
Doctors then must assess a patient for things like:
- When they began exhibiting symptoms;
- Underlying conditions like diabetes or heart conditions;
- The risk of developing a severe case of COVID-19.
Based on that, the doctor treating you may prescribe treatments like...
Remdesivir
Kumar said this is the most common drug administered to moderately or severely ill COVID-19 patients in the hospital. It’s administered over five days through an IV. Remdesivir doesn't kill the virus, instead it slows its development, Kumar said.
It’s one that was given to former President Donald Trump when he was treated for COVID-19 in October 2020.
Inhibitors
Kumar said some patients may be administered JAK inhibitors. This medication has some antiviral activity and alters how the immune system responds to COVID.
Interleukin-6 inhibitors may also be given to reduce inflammation. Both of these inhibitors can reduce the duration of symptoms and likelihood of death.
Supportive medicines and treatments
Depending on what a patient needs, doctors may order treatments like:
- Steroids for the inflammation that COVID-19 causes in the lungs;
- High-flow oxygen through the nose;
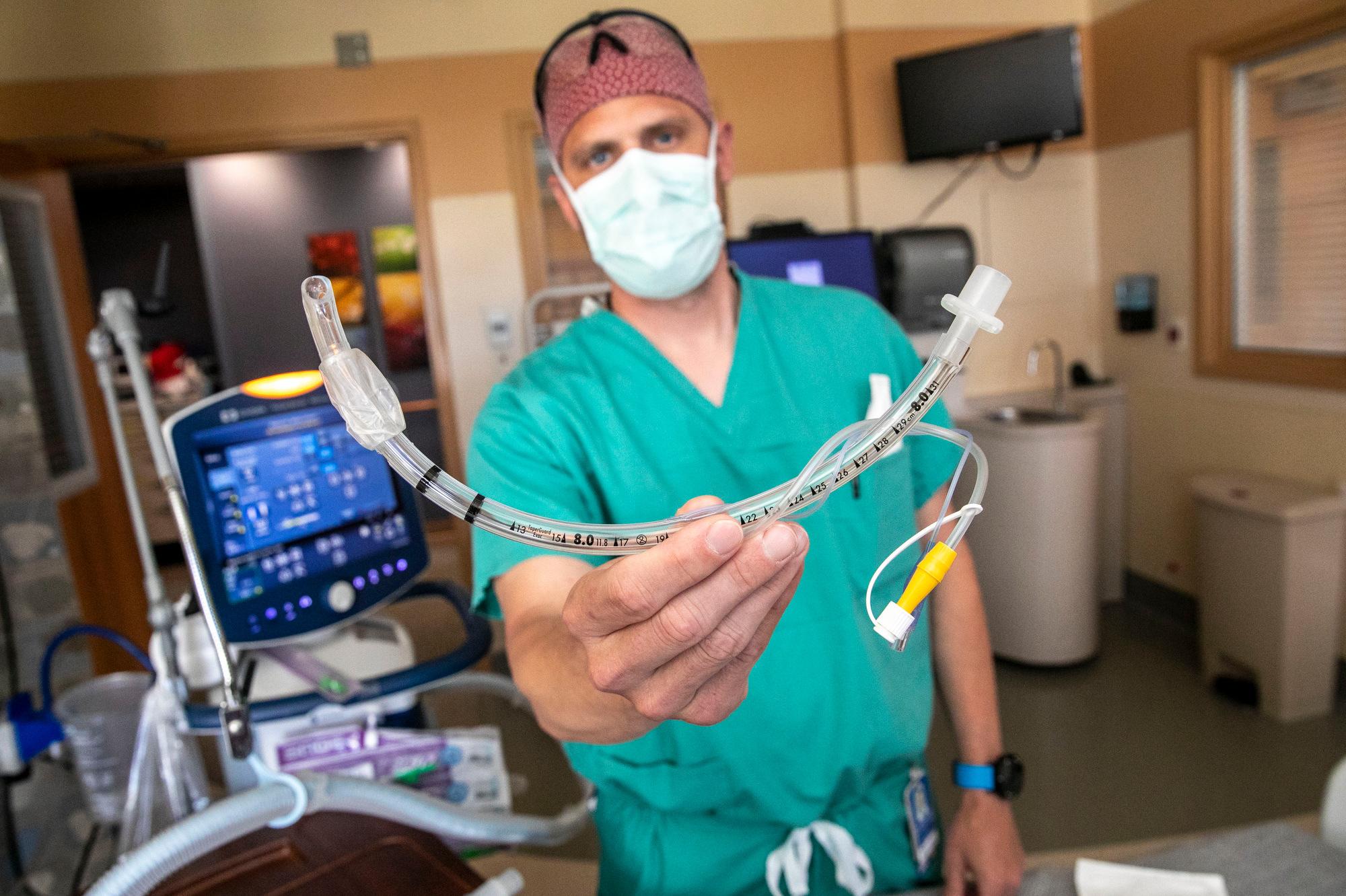
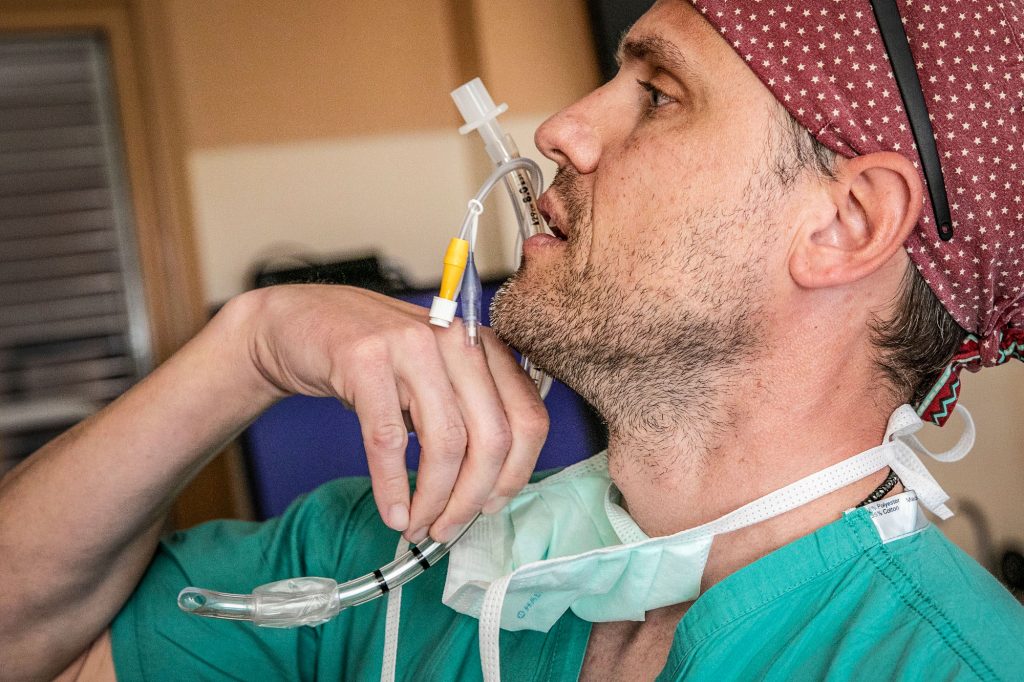
- Being connected to a ventilator, which includes placing a tube in the respiratory system, for the most severe COVID-19 cases.
Kumar said there are rare cases when a patient is connected to an ECMO machine, which circulates blood outside the body to get oxygen and allow the heart and lungs time to recover. This equipment, she added, is very uncommon and few hospitals have these machines.
One Colorado man who was recently released form the hospital, was connected to an ECMO machine for three months while recovering from COVID.
But surely there are antiviral drugs for COVID-19 available.
The FDA on Dec. 22 gave authorization to Paxlovid, a COVID-19 antiviral drug from Pfizer, that can be administered orally at home to anyone 12 years or older. But supplies will be limited, reports the Associated Press.
Merck also has a pill that could soon get authorization from the FDA.
Kumar said early data shows that Pfizer’s pill could reduce hospitalizations by up to 89 percent; the Merck option may reduce hospitalization by about 30 percent in high-risk patients.
But Coloradans can’t expect these drugs to be quickly delivered in large quantities if they are given approval by the federal government, said Dr. Eric France, the chief medical officer with the Colorado Department of Health and Environment.
The state would receive a small number of doses and that would grow based on demand and need, France said.
“We hope there’s a future state where they’re available like any other drug.” France said. “A physician would prescribe it, and the individual with COVID would pick them up in their pharmacy and take the five-day course and be better for it.”
Your best bet against COVID-19 is the vaccine.
Kumar said that if someone gets a severe case of COVID-19, they could theoretically receive the entire collection of therapies and treatments outlined above and still die.
“We’ve had breakthrough discoveries with the vaccines and the medications, but remember this virus is clever and it mutates,” Kumar said. “And when it mutates, it has the survival advantage. The variants could evade your immune system, could cause severe illness.”
That’s why, she said, step one to fighting COVID-19 is getting vaccinated because it can reduce risk of severe illness and death. She stressed that the therapies and medicines available may or may not work and they aren’t cures.
“We see that all the time in the hospital. We tried everything — still we couldn’t prevent you from getting on a ventilator or dying,” Kumar said. “We have people who tell us while they’re going on a ventilator ‘I wish I would have been vaccinated.’”
Editor's note: This article has been updated to reflect that two monoclonal antibody treatments are no longer being used because they are not effective against the omicron variant.
- ‘This isn’t just a number to me’: UCHealth chaplain reflects on the loss of more than 10,000 lives to COVID-19
- Colorado patients and providers alike are frustrated, angry and worried as COVID cases pack hospitals across the state
- Colorado COVID surge — and a staffing crunch — mean new crisis plans for hospitals









