
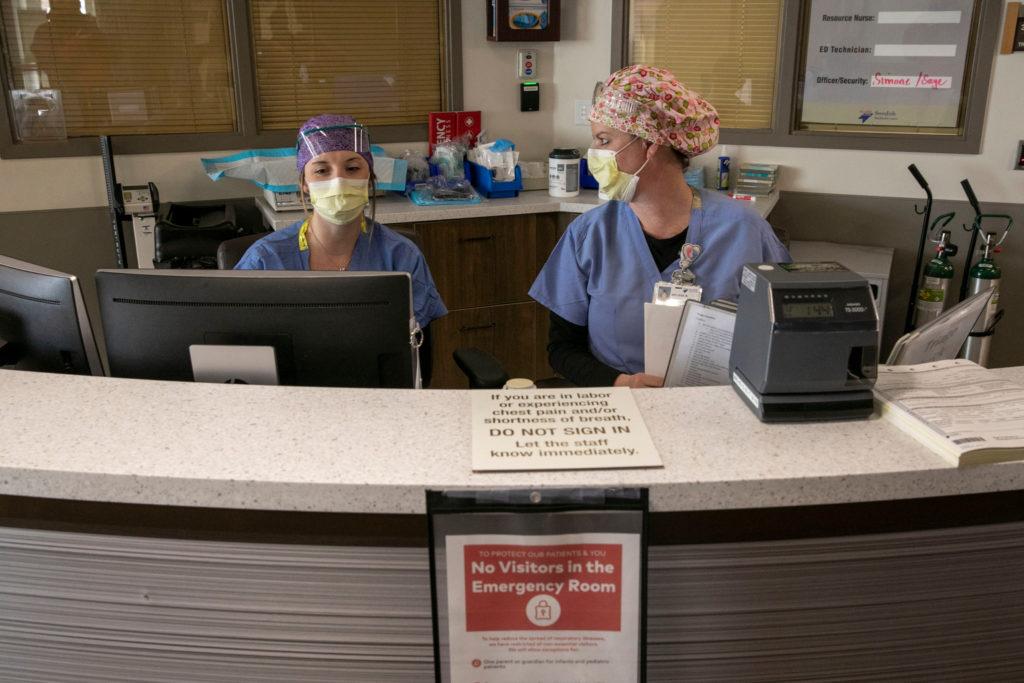
On a typical weekday afternoon, it would be standing room only in the waiting area of the emergency department at Swedish Medical Center. But there aren’t a lot of patients here these days. Coloradans are avoiding ERs like the plague — or a deadly virus.
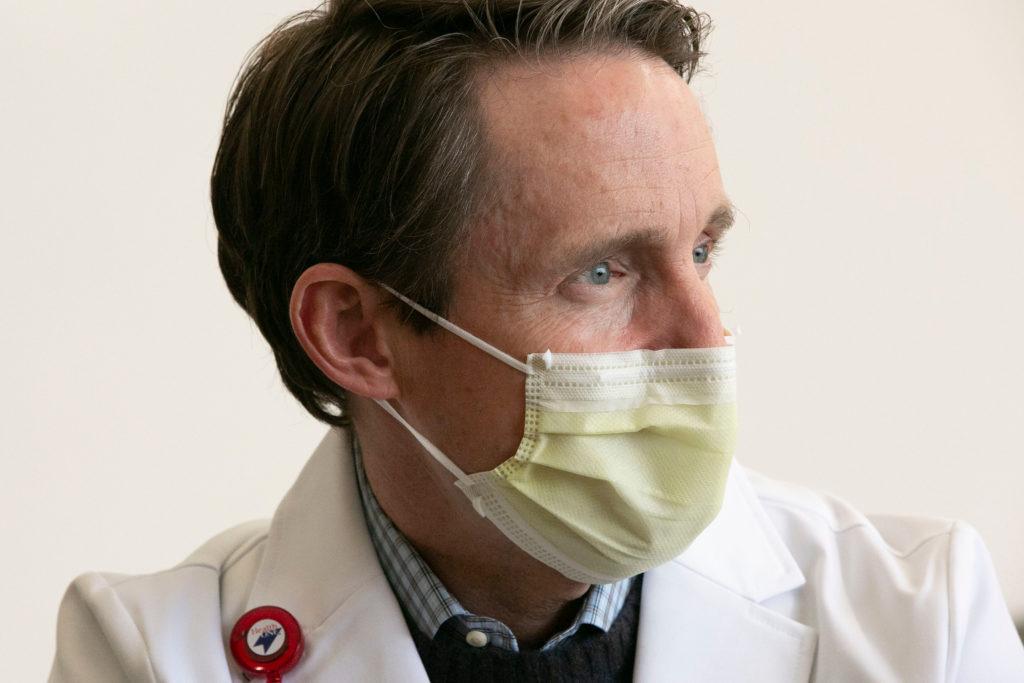
“We’re sitting in a lovely, clean, empty waiting room,” said Dylan Luyten, Medical Director for the emergency room at the Swedish Medical Center in south metro Denver.
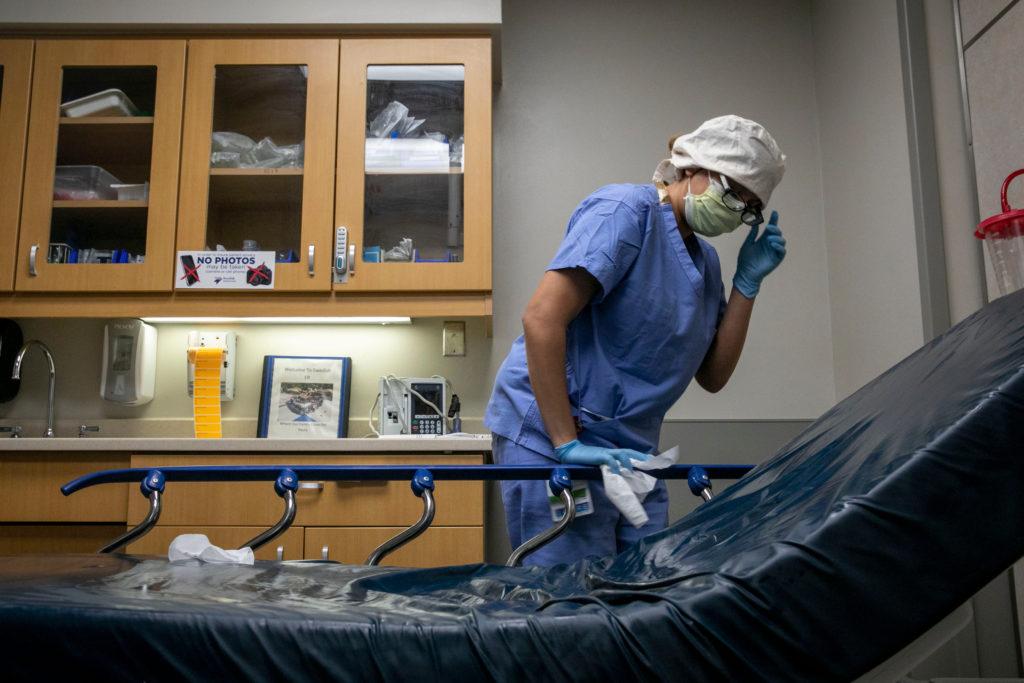
The room is as antiseptic as it is empty, with workers disinfecting the chairs and floors to protect anyone who does happen to walk in against COVID-19.
“At this time, we'd probably have a full waiting room of family members and patients and we'd probably have 10 or so people who are waiting to be seen,” said Luyten, who spent several months planning for a surge of coronavirus patients that was originally predicted to hit Colorado in March or April.
State researchers now predict that a peak in the number of hospitalizations due to the virus will come in May, though Luyten thinks the state has already passed its peak.
While many might imagine ERs across the state packed with sick, feverish, coughing patients, the volume of patients is way down at Colorado’s emergency rooms — about 30 to 40 percent down. Hospitalizations in the state are down too, in part because elective surgical procedures have been put on hold.
The numbers reflect nervousness about coming to the hospital and getting infected with the coronavirus. And many have heeded the words of Gov. Jared Polis, who at one point asked that if people think they have COVID-19, they self isolate unless they develop severe symptoms requiring them to go to the hospital.
“People should not be flocking to the emergency room unless they are in dire need of treatment,” Polis said in one of his earliest press conferences on the coronavirus at the beginning of March.
The problem is, ER doctors like Luyten say, the pandemic has led some people who are in need of treatment to stay away or at least hesitate to come to the hospital.
“I took care of somebody the other day who had a kidney stone,” Luyten said. "She'd been sitting in her car in the parking lot for a couple of hours, terrified to come into the ER because she thought she was gonna get sick or be taking a room [from] somebody else.”
Avoiding medical care can be dangerous, even fatal. Doctors fear patients are having strokes, complications from diabetes and other ailments, but aren’t coming to the ER because they’re worried about the virus.
Those concerns may have led Polis to offer a different message when he urged people to go to the ER if they need treatment.
“Some of you ... might be fearful about seeking out hospital care,” Polis said at a news conference Wednesday. “If you have symptoms like pain in the chest or dizziness [and] you would have called 911 or gone to the hospital two or three months ago, that should still be the way you operate today.”
Fear of getting COVID-19 isn’t the only reason people aren’t showing up at ERs lately, Luyten said. Another reason is there’s less crime, no bar fights and not a lot of ski injuries or car accidents right now.
Until a week or so ago, some of the patients who might have had broken bones or heart problems had been replaced in this ER by more coronavirus patients. But now Lutyten said, like other Colorado hospitals, the numbers have leveled off. Even Denver Health Medical Center — in the heart of urban Denver — reports its intensive care unit hasn’t yet been overwhelmed, though doctors there and at other ICU’s across the state say they remain busy with lots of very sick COVID patients.
In the past month or so, Luyten said he’s seen plenty of sick patients in the ER with COVID-19, many who ended up in the ICU.
“I had an 85-year-old gentleman the other day who was chronically ill, had multiple medical problems and lived in a nursing home,” Luyten said. “His wife had died the week before, presumably of COVID, his roommate in the nursing home had died a couple of days before, and he came in very, very ill and looking like he was dying.”
That man didn’t survive, and there have been other cases like his. Luyten said those cases are the ones that stay with him.
“I've seen people who were essentially well in the morning and were on a ventilator and actively dying by the evening,” he said.
Luyten is thankful hospitals haven’t been over-run and he credits Gov. Polis for stepping in early to impose social distancing restrictions.
Doctors and nurses still lack enough personal protective equipment, requiring caregivers to recycle masks they would normally throw away after a single use. And there are still worries about what the second wave of patients might look like if business as usual resumes too soon in the state.
Luyten remains grateful to Coloradans for mostly taking social distancing to heart and for all the food deliveries and words of encouragement. He and his colleagues might even admit to feeling a little underutilized and over-appreciated.
“What we're seeing right now is probably what success looks like, which is ... manageable, significant amounts of sick people with COVID,” he said. “None of our resources are being overwhelmed.”









