On the high plains, a vast area of Eastern Colorado, the concept of physical distance is a way of life. Driving 30 miles to the grocery store to stock up for a month is normal.
Now residents are counting on wide-open spaces to keep them safe during the worldwide coronavirus pandemic.
The Eastern Plains have seen just a few cases of the disease so far. But rural healthcare providers are anxiously tracking its spread from cities to outlying areas. They’re securing medical masks and calculating helicopter flight times to transfer extremely sick patients to larger facilities.
The Eastern Plains Healthcare Consortium could help. Several independent Plains hospitals, who had formed the Consortium a few years earlier, selected Banner Health, one of the largest nonprofit healthcare systems in the U.S. to become a member.
They will likely need to work together, because across their seven counties and more than 20,000 square miles stacked along Colorado’s border with Kansas, healthcare staffing is sparse.
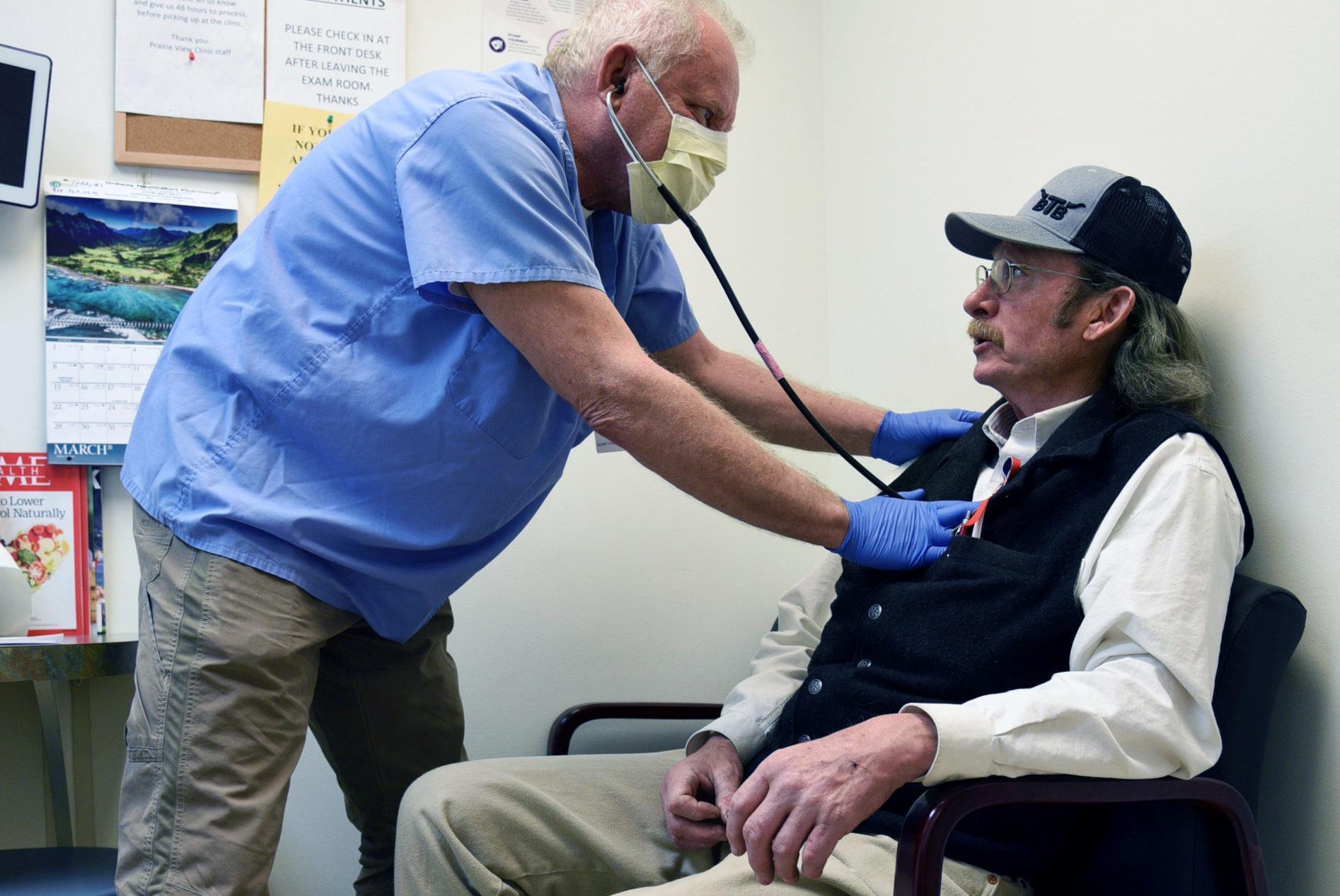
Dr. Kurt Papenfus is chief of the medical staff at Keefe Memorial Hospital in Cheyenne Wells.
“The problem is, right now, I'm the only doctor for 1,800 square miles, including this part of Colorado and part of Kansas,” he said. “It's got real potential to get really bad to where, you know, you have to decide who gets the ventilator and lives, and who doesn’t.”
Older adults, who are at the highest risk of severe symptoms from the new coronavirus, make up a large part of the population in these windswept counties. Many young people have left for jobs in the cities.
The shortage of doctors and nurses on Colorado’s Eastern Plains has been going on much longer than the current pandemic. They also lack the personal protective equipment they need. Now comes this virus that quickly spreads through close contact and on surfaces.

One ventilator, and few backup options
Stella Worley leads the hospital where Dr. Papenfus works in Cheyenne Wells. Keefe Memorial has just six beds. She says her team will be ready with several more if a surge comes.
“My number one job now is keeping staff well for the unknown,” Worley said. "A lot is expected of them. So, it would be disastrous if nurses got sick and it would be disastrous if providers got sick.”
For Worley, protecting the health of people in Cheyenne County is personal. She was born at Keefe Memorial, delivered by Dr. Jerome Keefe, for whom the hospital is named. She knows the challenges of providing care with few facilities spread out over huge territory.
“So, if the cities are inundated, then where can our people go?” Worley said. “If someone does get ill, we have one ventilator.”
Worley is worried about the potential sudden downward spiral of a COVID-19 patient and possible transportation options.
“We have a helicopter that can come in,” she said, “but if the helicopter is helping someone else, you're not going to get helicoptered very soon. There are only so many ambulances in the county. Where is there an available bed to take them? Burlington’s closest. Eads would be next and then we'd check Hugo.”
But each of those presents its own problems. First, they’re nearly an hour’s drive away in different directions. Hugo’s Lincoln Community Hospital has no ventilator, and it recently announced its first known positive case of COVID-19. In Eads, Char Korrell runs the Kiowa County Hospital District.
“We have no doctor,” Korrell said.
The small hospital uses telemedicine, where a doctor and nurse from South Dakota see a patient from Eads on a screen, with a nurse practitioner in the room.
“We have one ventilator,” Korrell said. “We’ve never had to use it. We could actually hook up two people that would be on high flow oxygen and if they needed low flow oxygen, we could hook up as many as four. It's scary to think that we would have more than that who would need it.”

A plan to swap patients with big city hospitals
In addition to running things in Eads, Korrell chairs the consortium of hospitals that formed last year. She says the partnership has already helped her hospital save thousands of dollars on regular supplies through group purchasing power.
She cites the collective leadership experience of the nine consortium CEOs as a key source of support and knowledge.
“During this crisis, we’ve been emailing almost daily,” she said. “Someone gets an update and then we forward that on, or we all get together and say let’s talk about this.”
The CEOs are brainstorming how and where to add beds, and maybe cots.
They also have ideas about how to work with Front Range hospitals during this pandemic, which might mean Eastern Plains hospitals wouldn’t have to handle the coronavirus on their own. They are offering to take in patients from the cities who do not have COVID-19 to get those vulnerable people away from the center of the crisis.
Korrell said, “If we have open beds, we could take those patients and get them back home without them ever having been exposed to the virus.”
In exchange, the Plains hospitals might be able to send their very sick COVID-19 patients to the cities. But even the cities are short on ventilators and other supplies and space they expect to need.
With Plains providers facing a shortage of equipment and beds, and the prospect of losing an entire medical staff if doctors and nurses get sick, Korrell says the self-reliance that’s required for living on the prairie can help. Growing up, she often heard stories from her grandparents about the Dust Bowl, which decimated the Great Plains in the 1930s.
“The resiliency that rural frontier people have gives people a stamina to go through kind of a long journey, a tough journey, being alone,” she said.
She grew up with skills that people in other parts of the state may be picking up for the first time during mandated social distancing.
“You learn to grow a garden and you learn to harvest that food and you learn to can and you learn to bake bread and then you store all of that for later. Or you share it with your friends, who don’t can, but need the food,” she said.
For people like Dr. Papenfus, the cities and plains are vitally connected. The Plains can’t just be an afterthought — especially during the pandemic.
“Denver, Boulder, Fort Collins,” Dr Papenfus said. “That's where everything's happening. That's where the political action is. Our ace in the hole is we're the farmers. We're the ones that feed Denver and Boulder, so they'd better pay attention to the rural people.”
Even before the current pandemic, rural hospitals in Colorado have been operating at a loss. They’ve been fighting for their lives. Now, they’ll keep doing that — while also fighting for the lives of people who get sick with the coronavirus.
CORRECTION: This story has been edited to reflect the correct sequence of events in the formation of the Eastern Plains Healthcare Consortium.









