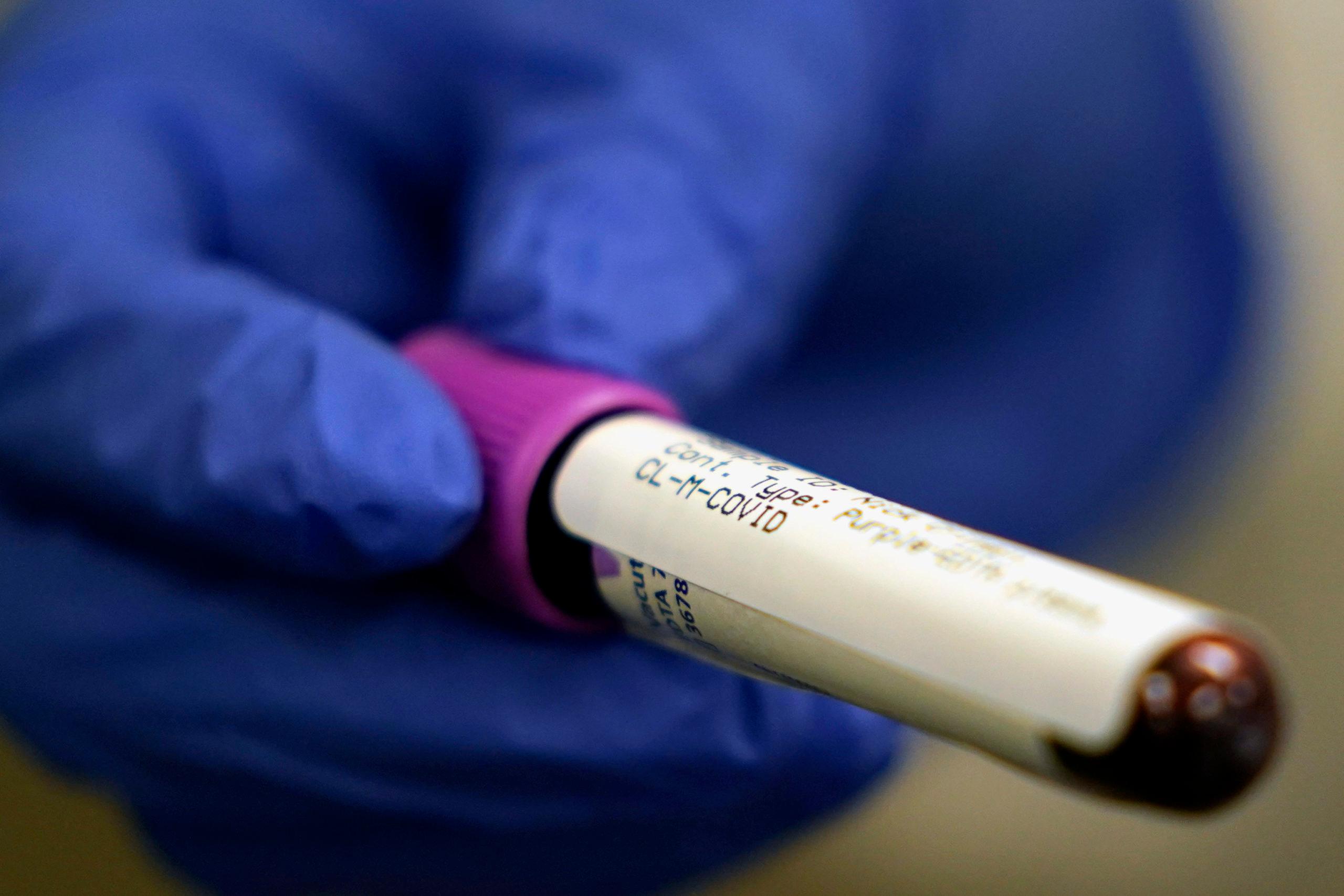
Colorado obliterated its record for COVID-19 cases in a day, with more than 2,100 reported Sunday, Oct. 25, as the coronavirus approached or surpassed records in all parts of the state, and rising intensive care occupancy created new concerns about capacity.
Before this past weekend, Colorado had never recorded more than 1,267 new cases in a day. Then came Friday, Saturday and Sunday, when the state recorded 1,604, 1,594 and 2,102 cases on consecutive days. Those also coincided with three of the busiest testing days in the state since the start of the pandemic in March, with a record 31,847 tests reported administered on Sunday.
The growth in testing was almost bound to lead to a growth in cases uncovered, but the percentage of tests coming back positive, a reliable gauge of the direction the pandemic is taking, is also growing, just not as dramatically. The 7-day average positivity rate has grown from 3.36 percent to 6.67 percent just in October. At the peak in April, when testing was scarce but the virus was pervasive, more than 22 percent of COVID-19 tests returned a positive result.
The current growth in cases and positive tests is occurring despite repeated admonitions from public health officials and Gov. Jared Polis that the pandemic is not yet behind the state and that mask-wearing, hand washing and social distancing remain critical strategies for keeping the virus in check and the economy open.
Polis will try again Tuesday, with a briefing for the state at 12:30 p.m. featuring patients who have survived the illness.
The growth in cases is being felt throughout the state. Mesa County in far western Colorado routinely reported weekly case counts in the single digits in April and May while much of the rest of the state reported much higher numbers and fears about hospital capacity. But as September gave way to October, even Mesa was feeling the coronavirus, with new weekly cases in triple digits, and more than 500 cases recently recorded over two weeks.
Hospitalizations for patients with confirmed or suspected cases of COVID-19 are also growing, though not yet anywhere near the peak hospitalization numbers recorded at the height of the pandemic in Colorado. More of a concern is the percentage of ICU beds the state is using, which is actually higher than at the peak of the pandemic in April.
Back then, about 65 percent of ICU beds were in use for all illnesses statewide, and the state moved to create overflow temporary hospitals in case the numbers continued to rise, though they ultimately weren’t needed. Today, about 79 percent of available ICU beds are in use, with many patients who have illnesses other than COVID-19.
That adds to officials’ concerns that as winter approaches, and ski tourists arrive, more people move indoors and cases of COVID-19 rise along with other illnesses, ICUs in the state could be overwhelmed.
Denver Health "selectively" postponed some elective surgeries that required a hospital bed that were scheduled for Tuesday and is closely monitoring the use of hospital and ICU bed space. The city warned residents Monday that a new stay-at-home order was possible if the positivity rate and hospitalizations did not turn around.
"What we are doing isn't working," the city tweeted to residents.
The state's data on cases was increased over the weekend by the addition of about 16,000 test results - negative and positive - from Kaiser centers that, due to a technical glitch, had not been recorded since the start of the month. But those were apportioned to the days on which the tests were reported to Kaiser, and should not have played a role in the record-setting case reports from the weekend.
The Colorado Hospital Association’s Julie Lonborg said hospitals are worried that if the ICU beds continue to fill, there won’t be enough specially-trained staff to work in them.
She said one reason more people suffering from other illnesses are now in the ICU than earlier, is that in March and April, officials began telling people to avoid hospitals to reduce the spread of the virus.
Officials have admitted that the message may have gone too far as patients with severe illnesses like heart attacks and strokes avoided care.
- Growth In Coronavirus Positivity Rates In El Paso County Could Mean More Restrictions
- New Phone App To Track Colorado Coronavirus Exposure Arrives
- As Coronavirus Cases Rose In Colorado, Outbreaks Did Too
- Colorado Is Entering A Dangerous Third Wave Of The Coronavirus Pandemic, Polis And Top Health Leaders Say
- Climbing Coronavirus Cases In Pueblo County May Lead To Loss Of Variances And More Restrictions
Lonborg said now hospitals are urging people to come back but some are coming back sicker because they’ve delayed treatment.
“Our message today is if you're experiencing warning signs of a heart attack or a stroke or don't wait to be seen,” Lonborg said.
Lonborg said another reason more people are in the ICU is that as people have started to socialize more, more people are getting injured in car- or work-related accidents, which has added to the number of critical care patients. And she said along with more COVID-19 cases, the colder weather also brings more respiratory illnesses that can turn into more serious health problems.
But Lonborg said there are reasons to be optimistic about how well hospitals and doctors can handle another spike. For one, they know more about how to treat the virus and now ventilate far fewer patients.
“That enables us to care for more and more of those patients,” Lonborg said. “It also makes it easier to turn other units and other beds into ICU [beds], because we're not dependent on ventilators with which to do that.”
Lonborg said in the spring, hospitals got better at figuring out how to reconfigure and expand other hospital units if they needed more ICU space. For example, they may use emergency room beds as temporary ICU beds.
“[Doctors in the ER are] used to caring for critically ill patients and sometimes you'll hold a patient in the emergency department until the timing is right to move them to the right bed or to the ICU.”
Some hospitals created ICU units exclusively for COVID-19 patients and used other units of the hospital for other patients who need critical care.
Lonborg said the hospitals also shifted patients to other hospitals if necessary. A very sick patient might be transported from a rural hospital without ICU beds to an urban hospital or, an urban hospital might send a recovering COVID-19 patient to a rural facility to recover.
Still, Lonborg urged people to take added precautions, particularly to keep socializing to a minimum and wear masks.
As for deaths from COVID-19, the state remains far from the darkest days of the pandemic in April where there were more than 30 COVID deaths a day. But those numbers have been rising as well.
While the state hasn’t recorded double-digit deaths since July, there have been 9 deaths recorded on two days in October, and the increasing hospitalizations could be an ominous sign that a growth in the number of deaths will follow.
Several counties have taken steps to re-institute restrictions, but all are counting on residents to react to the latest numbers and take action to prevent a return to April’s statewide shutdown.
In a release sent to its residents Monday, Pueblo pleaded for citizens to take the necessary steps to stop the spread of the coronavirus.
“There is a small window of opportunity over the course of the next few weeks to make improvements in Pueblo County’s numbers,” the release said. “Everyone plays a part.”
Denverite's Esteban L. Hernandez contributed to this report.
Editor's note: This story has been updated to clarify that only elective surgeries requiring a hospital bed and scheduled for Tuesday were postponed by Denver Health.








