
In an update on Nov. 5 at 12:30 p.m., Gov. Polis and state epidemiologist Dr. Rachel Herlihey said state data shows Colorado hospitalizations are at an all-time high of 894. The previous peak came in April 2020, at 888. State modeling suggests some counties have rates of spread as high as one in 100 contagious residents.
Colorado hasn’t turned the tide on its rising coronavirus spread, according to new data released by the state.
Virtually every gauge state and local health leaders watch closely is headed in the wrong direction. The three-day rate of positive tests jumped to 10.79 on Election Day, with the seven-day rate at 9.31. Doctors grow concerned about the spread of the virus when that figure hits 5 percent; the state has been above that since mid-October.
The number of Coloradans hospitalized with COVID-19 neared an ominous threshold the day after the election, approaching the peak first reached last spring.
A total of 847 patients who are confirmed to have the virus are now in the hospital. That number is expected to soar past the 888 reached in April within a day or two. The total patients confirmed or suspected with the virus is 970, according to data from the state health department, still considerably lower than the peak of 1,277 reached on April 9.
Testing has vastly improved since spring, but top health leaders say the coming weeks will be critical to containing the spread of the virus.
“It certainly is a worrisome milestone,” said Rachel Herlihy, the state epidemiologist. “I think at this point we probably have as much disease circulating in Colorado as we did at that peak.”
Eighteen counties have two weeks to lower their COVID-19 numbers
Colorado now faces serious headwinds in reining in the virus. Flu season has arrived. Thanksgiving and the winter holidays could drive coronavirus transmission upward unless families take steps to protect themselves.
That likely means the kind of restrictions last seen in some communities months ago, like curfews and limits on gatherings. And reduced capacity caps for businesses are coming down the tracks unless the trends change.
Colorado's top health officials said 18 counties now see transmission levels that could lead to the most restrictive level of response on the state’s colored dial: Stay at Home.
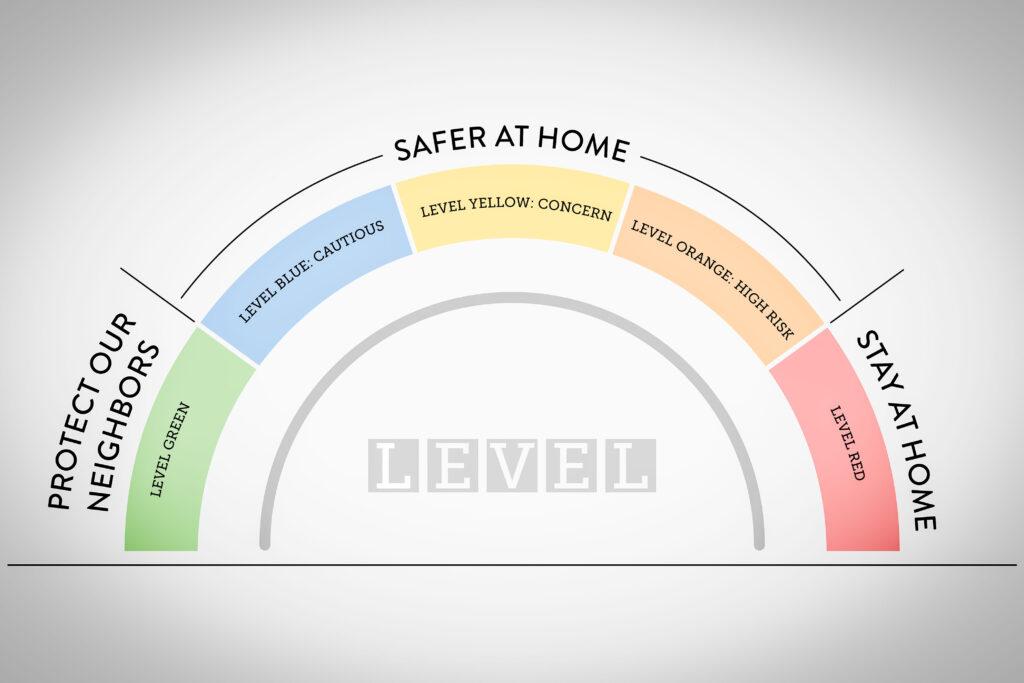
Dr. Eric France, the state's chief medical officer, said local leaders must put new restrictions in place starting now — including limits on gatherings and curfews, like the one ordered last week in Pueblo. “I would not be surprised in the next weeks if we see more of that in our state,” he said.
The 18 counties, shown in dark red on the state’s dial dashboard, are:
- Denver
- Douglas
- Adams
- Arapahoe
- El Paso
- Jefferson
- Broomfield
- Weld
- Morgan
- Sedgwick
- Phillips
- Washington
- Kit Carson
- Crowley
- Otero
- Pueblo
- Prowers
- Alamosa
France said counties have two weeks to take steps to reduce transmission. If they don't, the state may implement stay-at-home rules for them. “As long as these rates are going high, that will, unfortunately, be a real option,” he said.
The state health department has notified Broomfield, Boulder and Jefferson counties they would be moved to Orange status, one step away from Stay At Home. Broomfield and Boulder will make the shift at 5 p.m. on Friday, Nov. 6; for Jefferson, it’s Monday, Nov. 9.
France said communities and families can prevent a step up to more restrictive measures, which have big economic implications. “Of course the goal is to avoid the stay at home (order),” he said. “That's really what we're all working towards.”
“I think it's time for Colorado to really take seriously the level of disease transmission we're seeing and remembering the things that we need everyone to do right now,” said Herlihy. Those measures include the mantra of public health admonitions to wear a mask, practice social distancing, and limiting interactions with other households. She also urged Coloradans to get a flu shot, to limit additional illness and potential hospitalizations.
Coronavirus cases, hospitalizations and deaths are all up
COVID-19 deaths are also on the rise, with 16 deaths recorded Oct. 20th, the fourth day in the last couple of weeks with double digits. A few weeks ago, the state typically recorded three or four a day. The state also documented the sixth day in a row with more than 2,000 cases.
With hospitalizations rising, the number of deaths is expected to rise. “We are really just now starting to see an increase in deaths associated with this fall wave of illness,” Herlihy said. “I think unfortunately we're going to see many more deaths over the next couple of weeks.”
The rise in virus numbers across the board is “very disheartening,” said Dr. John Hammer, an infectious disease specialist at Denver’s Rose Medical Center.
“I think that we expected a rise in the winter when people started to have to be indoors more with more potential for exposure,” he said. “But I didn’t expect to see it quite this early.”
Public health officials, epidemiologists and frontline physicians said it seemed like multiple factors were driving what they are calling a “third wave” of illness in Colorado. Those include more people spending time indoors, where the virus circulates more easily when airborne, and more people joining gatherings outside of work or school.
Another issue: “COVID fatigue,” said Dr. Jon Samet, the dean at Colorado’s School of Public Health, who directs COVID-19 modeling for the state. He said many people are tired of “contending with all that we need to do.” He said his team had noted a “drop in transmission control at all ages, so I think we need a combination of doing better as individuals, coupled with some of the policy options.”
Samet also said it’s possible the seasonal change plays a role. “Perhaps the virus likes cold weather,” Samet said.
Largest outbreaks are in detention centers
Outbreaks, defined as two or more cases in a single business or other settings like a school, do not appear to be driving some of the case increases. The latest report has 66 new outbreaks in the state, far fewer than have been posted in recent weeks. The bulk of new outbreaks are in schools and other education settings.
Some of the largest ongoing outbreaks are still in corrections and detention facilities, including the GEO Group-run immigration detention center in Aurora, where 100 detainees have contracted COVID-19. Another 546 inmates and 37 staff at the state's Fremont Correctional Facility have caught the disease in an outbreak that began Oct. 12. There are 587 active outbreaks in Colorado now.
Despite all of the dire warnings, November 2020 is not April 2020. Doctors have learned a lot about how to treat COVID-19 in six months, said Dr. Richard Zane, chair of the department of emergency medicine at the University of Colorado School of Medicine.
“We are much better at recognizing critical illness, anticipating critical illness,” he said “We are much more confident in our ability to treat patients with COVID and have an understanding of what we need to do.”
Tested by the pandemic, Colorado hospital leaders and frontline providers have responded with what they describe as an unusual level of collaboration and innovation. The Colorado Hospital Association recently said it and the state’s hospitals and health system had created the Combined Hospitals Transfer Center, a system for moving patients between hospitals.
The center would be activated if the number of patients needing transfer outstripped the capacity of the hospitals. Transfers would be determined by data so patients get the care they need without overloading a particular hospital, the CHA said. The plan is if a hospital reaches capacity or can’t provide the needed level of care for a patient it would contact the center. The center will decide what hospital in the region or state can provide that care and has the capacity, while also considering proximity and patient preference.
“One of the best practices we learned from other states that have already responded to significant outbreaks was to stand up a statewide transfer center,” said Dr. Darlene Tad-y, CHA vice president of clinical affairs. “This will allow us to respond rapidly to capacity issues that a city or region of Colorado may face.”
By the end of December, models suggest ICU beds could hit capacity
A desire to not overload the health system guides many of the public health decisions. As of Nov. 4, 10 percent of hospitals anticipate staffing shortages in the next week and 4 percent anticipated a shortage of personal protective gear, the same percent said they anticipated a shortage of ICU beds.
If COVID-19 cases grow too sharply, every part of the system gets stressed, from nurses and doctors to supplies like personal protective equipment to scheduled surgeries.
By the end of December, ICU beds, which host the sickest patients, could hit their capacity, according to state disease modeling.
“It's the weeks more around Thanksgiving and beyond where now we're starting to be potentially concerned that COVID cases plus our traditional hospitalizations may overwhelm our staff and our beds,” France said.
In the worst-case scenario, hospitals would activate what is called “crisis standards of care,” a decision-making process to determine who gets what care first, should the number of patients outstrip the ability to care for them. Utah’s hospitals at the end of October said hospitalizations were so high they were considering a move to that posture.
“It's a constant concern,” said Dr. Anuj Mehta, a pulmonologist with National Jewish Health, who also works in Denver Health’s ICU. Mehta helped develop Colorado’s guidelines. “Obviously the concern decreased over the summer... And now, right, the concern is there every single day.”
Mehta said hospitals and other health care providers purchased more ventilators and made advances in deciding when to use them on patients.
“What we've learned...is that high-flow oxygen may be a better therapeutic modification rather than placing patients on a ventilator,” said Dr. Monique Butler, chief medical officer for Swedish Medical Center in Englewood.
COVID-19 patients in Colorado are less likely to go on a ventilator and spend less time on one than they did at the start of the pandemic, according to data released in October by Colorado’s hospitals.
Providers developed more “flex space,” rewiring ordinary rooms in the hospital so they could handle ICU patients. They also have learned kinds of treatments and medications worked best for COVID-19 patients.
“It doesn't prevent us from reaching crisis standards of care by any means, but it actually does give us a little bit of extra wiggle room,” said Mehta.
Since the pandemic hit in March, seven senior clinical leaders of each of the state’s health systems have been meeting on a near-daily basis to compare notes — something they’d never done before.
“Most of us have never met in person,” said Dr. Shauna Gulley, the chief clinical officer for Centura Health. “And the collaboration has been critical to advancing our learning quickly and critical to highlighting areas of risk” for state leaders.
The collaborative sessions are conducted over Zoom in the most 2020 fashion. It’s been critical to sharing knowledge and highlighting risk areas for state leaders, Gulley said, which will be useful as the system faces a new wave of cases.
Editor's Note: This story has been updated to reflect the fact that the state clarified that rates of spread of one in 100 contagious Coloradans are not statewide. Only some counties, including Denver, have rates that high. They have not named the other counties with similar rates.








